High Blood Pressure in Elderly People – The Definitive Guide
We can all agree that high blood pressure in elderly people (hypertension) is a condition that has to be treated. It’s dubbed “the silent killer” because it presents no symptoms for a long time until it’s too late to reverse its effects on vital organs. According to many doctors, prompt diagnosis and aggressive treatment for lowering blood pressure to normal levels are the right approaches.
What is considered high blood pressure in the elderly? Recent studies have suggested that slightly higher than normal blood pressure in seniors has a protective effect. This somewhat controversial new approach has shown that elevated blood pressure may indicate preserved heart function. Furthermore, it may actually protect the brain from dementia.
What Is Blood Pressure?
Essentially, blood pressure is the force that blood creates by pushing against the walls of the blood vessels on its way through the body. If you take a look at an elderly blood pressure chart, you can see that blood pressure is measured in millimeters of mercury (mmHg) and presented in the form of a fraction.
However, it is not a fraction, but two numbers, one over the other, representing systolic pressure (the upper number) and diastolic pressure (the lower number). Systolic pressure is higher because it’s measured when the heart contracts (beats), while diastolic pressure is measured when the heart relaxes between beats.
Signs and Symptoms of Hypertension in the Elderly
There is a big problem we need to mention here. And it involves high blood pressure in the elderly, usually showing no symptoms. As much as one-third of people who have high blood pressure don’t know that they have it. Often, the only way to diagnose it is by taking proper blood pressure measurements.
Fortunately, as you know, this is very simple, and it is one of the first things your doctor does when performing a physical exam. Therefore, if you regularly visit your doctor’s office, high blood pressure won’t be left undiagnosed. It’s recommended for people over the age of 21 to keep track of their blood pressure, and even more so for seniors.
When it comes to high blood pressure in the elderly, symptoms start to appear only at dangerously high levels. The symptoms of extreme hypertension can include:
- Intense headache
- Fatigue and confusion
- Problems with vision
- Difficulty breathing
- Chest pain
- Irregular heartbeat
- Pulsating in the chest, neck, or ears
- Blood in the urine
If you have any of these symptoms, you must see a doctor immediately. You could be having a hypertensive crisis that requires urgent treatment because it can lead to a heart attack or stroke.
How to Measure Blood Pressure
If you want to know how to control high blood pressure in old age, or in fact, any age, the first step is measuring it. There are a few ways to measure blood pressure, the simplest being with an electronic sensor that goes around your wrist. You can use it yourself, and it’s relatively accurate but not the most sensitive device out there.
What is the normal pulse rate for an elderly person? Regular heart rate varies from person to person, but a normal range for adults is 60 to 100 beats per minute. Additionally, low pulse rate and high blood pressure in the elderly are possible, especially if one’s hypertension is chronic. Namely, a low pulse rate may indicate a problem with the heart’s electrical conduction pathway.
There are special devices called ambulatory blood pressure monitors that record your blood pressure for the entire day and give the most accurate readings, but they’re more expensive, and they aren’t the standard practice yet. And, of course, there’s the good old blood pressure cuff and stethoscope.
Even more important than the device you use is the way you take the measurements. First of all, they have to be performed multiple times before making a definitive diagnosis. Second, the person has to be adequately prepared. What does that mean? For the most accurate readings of high blood pressure in elderly people, the patients should:
- Sit upright with their feet on the ground
- Relax for five minutes
- Not smoke or drink coffee for 30 minutes beforehand
- Use the restroom if they need to
- Wear short sleeves
There’s another thing that can influence the readings: some people feel anxious in a clinical setting and have elevated blood pressure only in the doctor’s office. You’ve probably heard of this—it’s called white coat hypertension. If your doctor suspects it, they will instruct you to measure your blood pressure multiple times at home and return with the findings. Ambulatory blood pressure monitors are also used in these situations.
What Is Normal Blood Pressure for Senior Citizens?
Your blood pressure fluctuates throughout the day. It’s lowest when you sleep but rises when you’re active, excited, or stressed out. This is normal. However, it’s stable most of the time and should be under 120/80 mmHg. Lower is better, but very low blood pressure for elderly people is also an issue because it can make them feel lightheaded and contribute to falls.
| Classification | Systolic pressure | Diastolic pressure | |
| Normal | Less than 120 | and | Less than 80 |
| Prehypertension | 120–129 | and | Less than 80 |
| Stage 1 hypertension | 130–139 | or | 80–89 |
| Stage 2 hypertension | 140 or higher | or | 90 or higher |
| Hypertensive crisis | Higher than 180 | and/or | Higher than 120 |
The values above are for the general population. What should an elderly person’s blood pressure be? Senior citizens differ from younger people in many ways. Age, frailty, other diseases, and the medication an older person takes all influence the approach to treatment.
When should we start treating high blood pressure for older adults? The most common threshold for beginning medications is 130/80 mmHg.
Overmedication of seniors is a serious problem. Treating multiple diseases, each with its own set of medications, can add up to over ten different pills per day, and every one of them can have side effects. Therefore, weighing the pros and cons of treating high blood pressure in seniors for every individual patient is necessary.
Another disease associated with old age is atherosclerosis. It reduces the diameter of the arteries leading to high blood pressure in older adults. The arteries also become harder and less elastic. Therefore, they can’t expand properly when the heartbeats, causing isolated systolic hypertension in the elderly. The diastolic pressure may remain normal, leading to a big difference between the systolic and diastolic pressures.
Too much medication can also cause orthostatic hypotension, that is, a temporary drop in blood pressure upon standing up. This can, in turn, lead to dizziness and cause falls. If overmedication is the cause, we have to rethink the doses. If the issue persists, consider getting a medical alert system.
On top of that, as previewed in the introduction of this article, for very old people (over the age of 80), elevated blood pressure can be a good indicator. How do we explain this? Well, hypertension in seniors means their heart is relatively strong to pump the blood with such force. Thus, high blood pressure can indicate a strong heart.
As for the second benefit, pumping more blood to an older person’s brain can ensure better oxygenation, which can protect the brain from developing dementia. So the blood pressure for an 85-year-old male who is otherwise in good physical condition can be a little elevated.
Medical professionals have known about these benefits for years, but don’t get it wrong; they are only true for very old people and for only slightly elevated levels. The causes of sudden high blood pressure in elderly adults must be identified and treated immediately, no matter the person’s age.
Also, seniors with diabetes and kidney disease have to aim for lower levels. What’s the bottom line? Simple math doesn’t work here. There is no one blood pressure threshold for starting medication, and an individual approach is vital.
What Are the Causes of High Blood Pressure in the Elderly?
High blood pressure patients are divided into two groups depending on whether or not the condition’s cause is known. In a great majority of cases of hypertension in the elderly, causes are not known. Blood pressure simply rises as we age, and many confounding factors contribute to its development. This is called primary or essential hypertension.
If specific causes of high blood pressure in elderly adults are identified—for instance, kidney disease or a tumor in the adrenal gland—this is called secondary hypertension. However, this type of hypertension is much less common.
What Are the Risk Factors?
Many risk factors contribute to high blood pressure development. Some can’t be modified, but most of them can. As a matter of fact, healthier life choices can prevent and treat hypertension without medications.
Is blood pressure affected by age? It certainly is, but let’s take a look at the other factors, too.
Unmodifiable Risk Factors:
- Age – Age-related risk factors can’t be modified; men over 45 and women over 55 have the highest risk of developing hypertension. Overall, hypertension in the elderly is common. The older the person, the greater the chance they will develop high blood pressure.
- Sex – As you can see, there’s a difference between the sexes. Men tend to develop high blood pressure earlier, while women are protected by estrogen until menopause. Afterward, the risk becomes the same.
- Race – Black people are most at risk of developing hypertension, followed by Caucasians, while Asians have the lowest risk.
- Family history – People with a family history of hypertension are themselves at risk of developing it.
Modifiable Risk Factors:
- Weight – Being overweight is a considerable risk factor for developing hypertension; losing even ten pounds can lower high blood pressure in elderly adults. Following that, you should aim for a healthy BMI.
- Diet – Eating plenty of fruits and vegetables, low-fat dairy, eggs, and lean meats will help you lose weight and lower your risk of developing hypertension.
- Physical activity – A minimum of 30 minutes of daily aerobic physical exercise is proven to be beneficial for preventing hypertension.
- Smoking – Tobacco smoking temporarily elevates blood pressure and damages the arteries in the long run, leading to high blood pressure, among many other adverse effects on the body.
- Salt intake – Salt (sodium) keeps water in your bloodstream and may become one of the causes of hypertension in the elderly. Limit your salt intake as much as possible and avoid processed foods that contain high sodium levels.
- Alcohol consumption – Two drinks per day for men and one drink per day for women has a positive effect on blood pressure levels, but don’t drink more than that because excessive alcohol consumption will have a negative impact on your blood pressure.
- Stress – Exposure to long-term stress raises blood pressure. Find ways to manage your stress and cope with problems instead of delaying them.
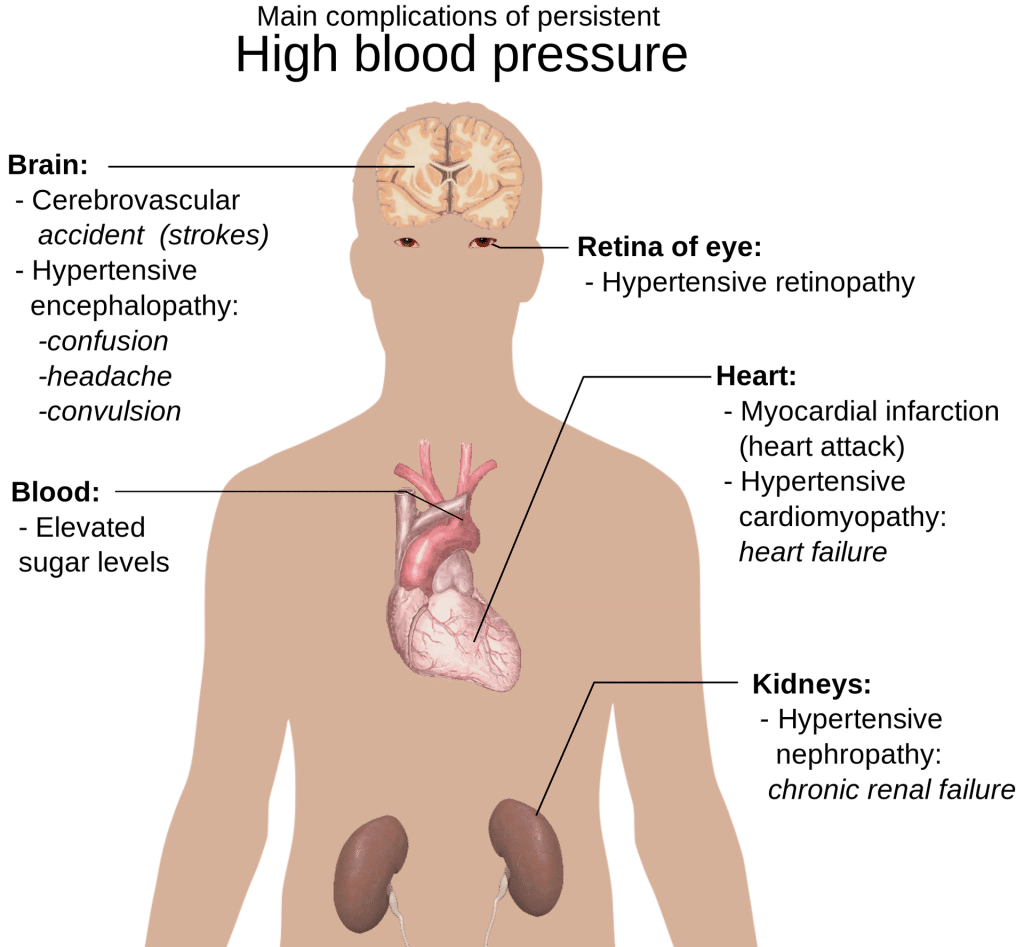
Complications of Hypertension in the Elderly
Untreated high blood pressure in older people causes some potentially life-threatening complications. While most of these problems won’t present themselves until old age, there aren’t complications of hypertension only in elderly people. In fact, more and more young people have hypertension, so diagnosing and treating it on time is crucial for preventing the following problems:
- Enlargement of the heart – When blood pressure is high, the heart has to pump harder, and just like any muscle, it grows to compensate. Paradoxically, this thins its walls and eventually weakens it, so the heart decompensates, leading to heart failure.
- Hardening of the arteries – The arteries harden when the high blood pressure in elderly adults isn’t treated for years. The damage occurs in all vital organs and throughout the body, but especially in the heart, brain, kidneys, and legs. That can compromise the blood flow to these parts of the body and cause a heart attack, a stroke, kidney failure, or amputation of the leg.
- Kidney failure – The same mechanism causes the arteries in the kidneys to become narrow, which damages their function. Kidneys are the primary organs for controlling blood pressure by eliminating excess water from the body. So we may have the chicken and the egg situation where we can’t determine whether hypertension caused the kidneys to fail or kidney failure increased the prevalence of hypertension in elderly patients.
- Aneurysms – Just like the heart expands under pressure, parts of blood vessels do, too, leading to little bulges in them that have thin walls (aneurysms). They tend to form on the aorta or the arteries in the brain. If an aneurysm bursts, it can lead to death in a matter of minutes.
- Vision changes – Damaged blood vessels in the retina can burst or bleed, which may cause vision changes and lead to blindness.
COVID-19 and High Blood Pressure
If you have hypertension, you should take even more care of yourself during the pandemic. According to studies, people with high blood pressure have an increased risk of:
- Getting COVID-19
- Showing worse symptoms
- Dying from the infection
In other words, the link between high blood pressure and the coronavirus is more than apparent. Astoundingly, an impressive 30%–50% of the COVID-19 patients in the hospitals of China and the US had high blood pressure as a pre-existing condition.
When it comes to the relationship between high blood pressure and COVID–19, it’s important to note that people with hypertension or other health issues have a weaker immune system, putting them at significant risk of contracting the virus.
Management of Hypertension in the Elderly
We can treat moderately elevated blood pressure levels (prehypertension) in the elderly by making simple lifestyle changes. This should be the first step before we resort to drugs. The following changes can be enough for some seniors to put their hypertension under control:
- Adopting a healthy diet with a limited sodium intake
- Losing excess body weight and maintaining a healthy BMI
- Being physically active every day for at least 30 minutes
- Quitting smoking and limiting alcohol consumption
Blood Pressure Medications
Sometimes making the changes mentioned above isn’t enough to lower high blood pressure in elderly people to acceptable levels. We then have to resort to pharmaceutical options. More often than not, two or more medicines have to be taken daily. They will keep blood pressure down but cannot cure hypertension. It is also essential to take the pills as your doctor prescribed them and take them every day at the same time.
The most common medications for treating high blood pressure in older adults include:
- Diuretics – These pills eliminate excess water and salt from the body via the kidneys. By reducing the volume of fluid in the blood, they lower blood pressure. They are often prescribed together with one of the following medications or combined in a single pill.
- Beta-blockers – Hypertension in elderly treatment options don’t end there. Beta-blockers reduce blood pressure by making the heartbeat slower and less vigorously, which, in turn, decreases the pressure on the blood vessels.
- ACE inhibitors – Angiotensin-converting enzyme inhibitors reduce the production of the hormone angiotensin, which causes blood vessels to constrict and elevate blood pressure. They also reduce the stress on the heart.
- Calcium channel blockers – Calcium has multiple functions in the body, and one of them is to enable the contraction of muscles. By preventing it from entering the muscle cells of the blood vessels and the heart, these pills relax them and lower high blood pressure in seniors.
- Angiotensin II receptor blockers – They target the same hormone as ACE inhibitors, but instead of preventing its creation, they stop it from working. When it comes to blood pressure in the elderly, guidelines recommend blockers for patients who don’t tolerate ACE inhibitors because this mechanism has fewer side effects.
- Alpha-blockers – Unlike beta-blockers, these pills target the blood vessels, causing them to expand, which reduces blood pressure.
- Alpha-beta blockers – They combine the effects of alpha-blockers and beta-blockers.
Conclusion
As you can see, the treatment for hypertension in elderly people is a complex issue. We have to take into consideration multiple factors and not just the generic threshold for high blood pressure in otherwise healthy adults. Every senior’s health has to be observed as a whole, and treatment needs to be adapted to every person’s unique needs.
FAQs
What is a normal blood pressure reading for a 70-year-old woman?
The ideal blood pressure is now 120/80 mmHg, both for seniors and younger adults. That said, high blood pressure for seniors starts at hypertension stage 1, ranging from 130–139/80–89. Moreover, if the blood pressure falls below 90/60, it is considered to be too low.
What are the new blood pressure guidelines for seniors?
Normal blood pressure is considered to be 120/80 mmHg, both for young adults and seniors. That’s according to the latest hypertension in elderly guidelines. Also, it’s crucial for seniors to monitor their blood pressure.
Does COVID-19 cause blood pressure spikes?
Recently, Livongo, a company specializing in health monitoring devices, carried out research on COVID-19 and hypertension. According to its findings, more people experienced hypertension in response to the pandemic. More specifically, before the pandemic, 62% of the Livongo members had high blood pressure, compared to 68% recorded in early April 2020.
How many elderly in the United States have hypertension?
Based on the US National Health and Nutrition Examination Survey, 70% of adults over 65 have high blood pressure. Even though older people have the highest prevalence of hypertension, treating hypertension in the elderly still poses numerous problems. That’s why we should raise awareness and monitor the blood pressure in the elderly on a daily basis.
How is a sudden blood pressure rise in the elderly life-threatening?
High blood pressure emergency is when your blood pressure is over 180 (top) or 120 (bottom). More specifically, it’s a life-threatening emergency with impending target-organ damage in the kidney, heart, large blood vessels, and brain. In such patients, severe conditions are suspected.
Why is hypertension common in the elderly?
As people get older, their vascular system undergoes changes. In fact, there’s a decrease in elastic tissue in the arteries, making them stiffer, leading to the increase of high blood pressure. But, age isn’t the only reason for high blood pressure in elderly people. Other factors include unhealthy lifestyle, genetic factors, and medications.





Thankyou really heiped to put things in perspective. I am 83 and very active playing tennis 6 hours a week suffer from white coat syndrome so doctor trying to put me on medication; which I now see is not necessary. BP 135/80 average taken using Omron machine.
do supplements and coffee raise blood pressure?
I was wondering if a spike in the blood pressure could be if 72-year-old woman got a infection in her mouth would that possibly raise her blood pressure a little higher than usual. Also is it good if the person is in pain from an infection to take a hydrocodone that they’re prescribed it to control the pain but also possibly bring down the blood pressure or would that make it increase the blood pressure that is?
Does an infection in somebody’s mouth raise their blood pressure. Also if somebody takes therw prescribed hydrocodone for pain would that help bring down the blood pressure?